
Research Articles
Interdisciplinary work: essential for optimising hearing implant outcomes
Instituto Nacional de Otología García Gómez, Bogotá, Colombia.
 OPEN ACCESS
OPEN ACCESS
PEER REVIEWED
PERSPECTIVES
Abstract
Technological advances and expanded indications for cochlear, bone conduction and brainstem implants have led to a significant increase in the number implant users, along with an increase in the number of professionals involved in the different phases of the process. At the same time, there is a tendency for professionals from different disciplines to work independently of their colleagues, focused on achieving their specific objectives. Hearing loss interventions not only have an impact on sound perception but on nonaudiologic factors too, including a person’s cognitive status, social interactions, family and work environment and many other factors, all of which play a major role in the wide variability of outcomes. As a result, comprehensive patient care is clearly needed.
Keywords
Implantable devices, comprehensive patient care, hearing loss.
Clinical implications
This article reflects on the importance of approaching hearing implant management from an interdisciplinary perspective, understood as the active collaboration of professionals from different disciplines and fields of action but with a common goal, which is to take maximum advantage of the auditory information received through an implant to improve the recipient’s quality of life. With so many professionals involved in the different phases of the implant process, the relevance of communication and cooperation is analysed, from diagnosis and treatment decision to post-implant rehabilitation.
Received: 04.10.2022 Reviewed: 06.11.2022 Acepted: 16.11.2023 Published: 09.04.2024
Edited by:
Helia Relaño-Iborra
Rochester University, EE.UU.
Technical University of Denmark.
Raúl Sánchez-López
Institute for Globally Distributed Open Research and Education (IGDORE).
Reviewed by:
Mariana Maggio De Maggi
Phonak Pediatric Program, España.
Marta Núñez
Hospital Universitario Virgen de las Nieves, España.
Faustino Nuñez Batalla
Hospital Universitario Central de Asturias, España.
Introduction
For audiologists who started their careers many moons ago, implantable hearing devices are the “miracle” that we once dreamed of. Frustrated and impotent, we used to be faced with guiding parents and patients themselves through a diagnosis of profound bilateral hearing loss, sharing their distress as we broke the unexpected and often devastating news, aware of the paucity of options that we could offer to help our patients hear.
The impact of severe to profound hearing loss is readily appreciated when one considers the intricate connections between hearing, language, the brain and emotions. The sense of hearing fundamentally facilitates communication, fosters social interactions, and supports cognitive tasks (WHO, 2016). It is essential for linguistic and communicative development. Even moderate hearing loss significantly affects speech and language development, causing academic and social difficulties and other long-term consequences.
The huge impact of severe to profound hearing loss can now be significantly reduced by early, effective interventions that provide individuals with adequate access to sound. The development of cochlear implants just over three decades ago opened a window of hope; we were finally able to offer patients the possibility of access to speech sounds in an increasingly efficient way. The positive impact of these interventions on our patients is a constant source of wonder. We have been privileged witnesses of a baby’s smile in response to hearing its parents' voice for the first time and we have shared the tears of joy of people hearing their name pronounced again, after living long years of silence due to hearing loss. By our patients’ side, we have experienced the amazement of hearing the rustle of clothes or the wind gently blowing the leaves on a tree.
The hearing implants available today bring hope to a diagnosis of hearing loss, regardless of its severity and type. Technological progress gives these devices increasing capabilities to efficiently translate acoustic signals into electrical or vibratory codes that the brain can interpret accordingly. Sound processing strategies incorporate algorithms that clean up the input signal for users, helping overcome the inherent limitations of a device with a small number of electrodes designed to reproduce the work of thousands of hair cells and nerve fibres in a healthy ear. And wireless connectivity, which forms part of our daily lives, is also integrated in sound processors, allowing them to connect seamlessly with a wide array of electronic devices.
Yet despite such significant technological innovations, the outcome is sometimes suboptimal. In addition to these innovations – ever faster data processors, signal filtering with pre-processing algorithms and smart microphones that adjust to different listening environments – other factors play a decisive role in the hearing outcome. Hearing loss has complex implications going beyond the mere perception of sounds, to the extent of even affecting brain development. Clearly, the problem cannot be addressed solely by simply amplifying sounds or replacing them with electrical impulses, despite their efficiency. Nonaudiologic factors, including a person’s cognitive status, social interactions, family and work environment, and a long list of other factors, play a major role in the widely varying outcomes of implantable devices. All these factors make comprehensive patient care paramount.
Subspecialties or comprehensive care
Health care professional practice is currently shifting between the opposing tendencies of promoting subspecialties to address each specific disorder and providing comprehensive care of a person as a whole. The first focuses more on treating isolated organs or functions and the second considers the human body as an organism made up of various systems interacting and cooperating with each other.
These two tendencies can also be found in the field of hearing implants. When cochlear implants first appeared, a multidisciplinary team was considered an essential requirement and worked actively from the preoperative stage onwards to decide whether the cochlear implant candidate would benefit from the new technology, taking all aspects into consideration. The teams were comprised at a minimum of an ENT specialist, an audiologist, a speech therapist, and often a psychologist (Parikh et al., 2004; Cooper 2006; Kim et al., 2010). Since then, the number of health care professionals working in hearing implant-related specialties has increased exponentially. Conversely, in some countries, the number of established implant groups has fallen, and the implant candidacy process is often managed by professionals working in isolation, such that the audiological evaluation is performed by an audiologist who has no direct communication with the ENT specialist or otologist who evaluates the suitability of the ear to receive the implantable device. In turn, the speech therapist in charge of the individual’s rehabilitation is sometimes not part of the decision-making process for the implantation procedure, never interacts directly with the otologist and sometimes not even with the audiologist (Ramos Macias et al., 2016; Warmer-Czyz et al., 2022). Furthermore, the professionals making the diagnosis and managing the candidacy process sometimes hand over to others for the device programming and aural rehabilitation. As a result, there may be no treatment plan that covers the perspectives of all the disciplines involved, and therefore the professionals from each discipline work alone, focusing on their own highly specific objectives. In some countries, this workflow has developed as a consequence of health care system policies.
Our view, which we invite readers to reflect on, is that interdisciplinarity should be recovered or introduced as a working model for managing hearing implant recipients, with the common goal of optimising the device’s benefits, which, consequently, will help improve the overall quality of life of our patients to the greatest possible extent.
Teamwork in health care
Advances in technology and in health care system organisation have changed the way heath care services are delivered, transitioning from a model of working in isolation to one comprised of a complex network of providers and professionals. Team-based health care refers to the provision of health services by at least two health care providers working collaboratively to accomplish shared goals (Babiker et al., 2014). The importance of teamwork in health care provision has gradually gained recognition and it is now very rare for patients to be seen by a single professional (Dihn et al., 2019, Rossen et al., 2018). Health services today require the cooperation of an array of practitioners from different disciplines.
The effectiveness of these teams depends on many factors, including the type of team, the characteristics of the team members, clear roles, leadership and commitment, and effective communication. In turn, barriers that hinder effective teamwork in health care include hierarchies, the individualistic nature of many health care disciplines and instability of team members (Rodriguez et al., 2021, Schmutz et al., 2019, Zajac et al., 2021).
The way in which the intervening disciplines interact defines the type of work team. Teams are mainly distinguished by their approach to the disciplinary perspectives and cooperation among the team members, as summarised in Table 1 (Roderick, 2010).
Table 1. Types of discipline relationships
DISCIPLINE RELATIONSHIP |
DISCIPLINARY PERSPECTIVES |
INTERACTION TYPE |
POINT OF VIEW |
MULTIDISCIPLINARY |
Separate perspectives, with individual objectives in each discipline |
Each discipline provides a specific, independent service with limited interaction |
A single study object from the point of view of several disciplines |
INTERDISCIPLINARY |
Common perspectives with shared but identifiable objectives for each discipline |
Each discipline contributes its specific skills and competences in a joint and coordinated way; there is integration and synthesis of disciplines |
Combines the viewpoints of several disciplines |
TRANSDISCIPLINARY |
A shared, single perspective |
Involves disciplines from outside the health care field working together under a shared conceptual framework. |
Combines the different viewpoints of each discipline |
In a multidisciplinary team in the health care field, each health care professional treats patients independently and shares information with the other team members, while the patient may be a mere recipient of care (Bernad-Bonnin et al., 1995, Choi et al., 2006).
A team is considered to be interdisciplinary if it is composed of different disciplines working towards a common goal, each contributing specific knowledge, skills and competencies (Greiner & Knebel, 2003), and if it promotes effective collaboration among professionals and facilitates a holistic approach to meeting patients' needs. The outcome is an integration of knowledge that can even create new disciplines.
Transdisciplinary teams in health approach the natural, social and health sciences in a humanities context, and in so doing, transcend each of their traditional boundaries by providing holistic schemes that subordinate disciplines, looking at the dynamics of whole systems. It is a methodology used in particular to resolve complex problems involving heterogeneous domains such as public health challenges or global climate change (Soskolne, 2000, Choi et al., 2006).
In the field of cochlear implants, different approaches range from individual and isolated work to interdisciplinary teams working with a patient focus. Transdisciplinary teams are rare, however, except in large hospitals or institutions.
An unequivocal symbiotic relationship exists between the fields of otorhinolaryngology and audiology, and likewise between audiology and speech therapy. The need for coordinated work among these three disciplines is therefore easy to defend in the management of patients with hearing loss. However, other professional areas, such as engineering, biomedicine, neurosciences, education, psychology, acoustics, and many others, are also directly or indirectly involved in hearing implants, and the interaction of these areas has contributed to the state of the art of these devices. This article focuses on the fundamental teamwork that must take place among the ENT specialist, audiologist and speech therapist, without taking away the merit of other professionals.
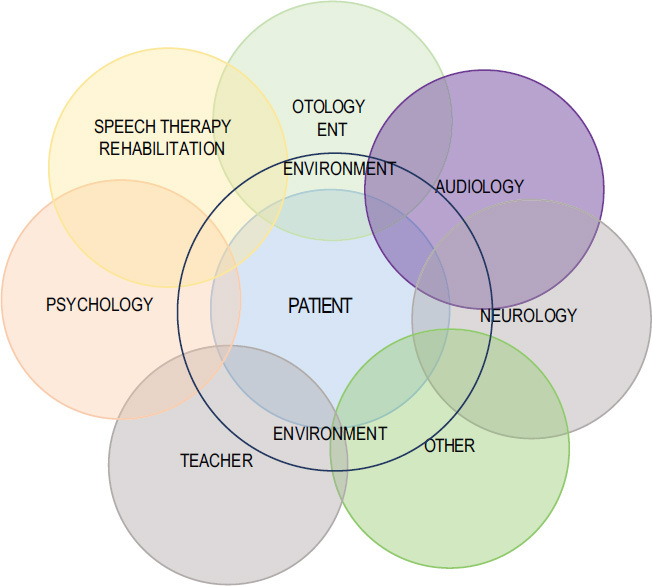
Effective and harmonious interdisciplinary work should have a defined framework of generic competences (attitudes and values) and specific competences (areas of knowledge) to facilitate a holistic approach, which in turn will undoubtedly result in better auditory performance and well-being of people with hearing loss, who are our focus of attention. By defining the competencies involved, the roles and responsibilities of each team member can be clearly established and mutually respected. Assertive communication is paramount among team members in order to plan the work to be carried out and resolve problems when they arise, acknowledging the importance of analysing situations from multiple perspectives. Figure 1 illustrates the key members of an interdisciplinary cochlear implant team. (Some disciplines may be known by other names in some countries.)
Figure 1. Interaction between the different stakeholders involved in the cochlear implant process
In the specific field of cochlear implant work, it is universally agreed that listening through an implant is clearly a different experience from acoustic hearing in a normal-hearing person. While a healthy auditory system contains thousands of hair cells that have the ability to code tiny spectral and temporal differences, leading to a high-resolution representation of the auditory information in the environment, cochlear implant systems have only a small number of electrodes available to represent auditory signals, resulting in a coarser representation of the complex and dynamic acoustic signals found in speech and music. In situations where there is a single sound signal, for example, when listening to one person speaking in a quiet environment, the healthy brain compensates for the lack of redundancy in the signal received and cochlear implant users generally perform well (Clark 2013, Boyle 2019). However, when the signal is degraded by the presence of other competing sounds or reverberation, or other challenging conditions, most individuals have noticeable difficulty and, in many cases, very poor performance (Dorman et al., 2017, Zaltz et al., 2020).
These difficulties occur regularly, albeit to a highly variable degree in different patients, and have triggered a search for options across different disciplines to optimise the devices’ benefits in terms of their design and improvement to the acoustic cues transmitted by the implant. Surgeons try to improve their vision and reduce trauma on electrode array insertion; audiologists use programming maps to promote the best possible representation of sounds by adjusting them to the individual’s required current configuration; and speech therapists seek to provide the necessary strategies for patients to adapt to and functionally use the information transmitted by their implant.
By following the principles of interdisciplinarity, these efforts can be combined and the different disciplinary angles can target a common goal. This synergy has been particularly relevant in recent technological advances in devices, when interprofessional discussions take place among physicists, engineers, surgeons, audiologists and other professionals about device limitations and needs. The diverse professional angles have led to solutions in device design and signal processing that have in turn resulted in better performance among users.
Yet communication among a surgeon, audiologist and speech therapist is sometimes absent, may be one-way only or lack fluidity and sometimes professionals forget that interdisciplinary discussions should be “conducted with equity, mutual respect, be void of personal interest and be focused on the patients’ interests” (Ysunza, 2014). Furthermore, professional interaction should be present at every stage of hearing device implantation. The decision-making process for an implantable device should start with an open discussion about surgical and nonsurgical treatment options, their possible outcomes, the specific challenges of the individual being treated and the choice of ear in the case of unilateral implants. These discussions become feasible in an interdisciplinary implant group setting. However, an ENT specialist sometimes knows about a patient's hearing only in the context of audiometry graphs or electrophysiology study curves. An audiologist, in turn, often first sees a patient for the initial implant activation, unaware of information that could guide the programming process, such as operating theatre notes describing electrode array insertion difficulties or partial insertion. An audiologist who is present in theatre and follows up the patient afterwards will have first-hand knowledge of the intraoperative measurements of implant integrity and function, but if a different audiologist follows up, they rarely receive this information. Likewise, an audiologist should report back regularly to the ENT specialist on progress, difficulties, unexpected changes in electrode impedances, extra-auditory stimulation and any other findings during programming sessions that require attention.
On-going, frank and respectful communication is also vital between a patient’s audiologist and speech therapist, while respecting their specific roles and responsibilities. Having a speech therapist present in person at implant programming sessions is extremely valuable, especially during the initial stages among paediatric patients. Since speech therapists often work with children, their presence not only reassures the child and parents, but they can also give valuable insights on their behaviour to guide the audiologist in the behavioural assessment of the specific current requirements of the different electrodes, which is essential in the programming process. Two-way communication and feedback between the two professionals makes a major difference to a patient’s progress. Before a programming adjustment session, an audiologist will benefit hugely if they receive information from the speech therapist about a patient’s perception of different sounds, details of possible phonetic confusions that can be fully or partially corrected by programming, progress in language and communication skills, their opinion on family collaboration, the child's interaction at school, and many more aspects that a speech therapist knows in more detail than the audiologist. In turn, the audiologist's feedback for the speech therapist is also paramount: they can provide details about the stimulation parameters used by the patient; detection thresholds achieved by the patient and then verified with free-field audiometry; specific findings on reactions to supraliminal stimuli such as undesired facial stimulation; discomfort with loud sounds; and results of speech-in-noise discrimination and speech perception in silence tests. Joint, coordinated teamwork affords more possibilities of optimising programming maps more accurately and precisely, while adjusting to individual needs, and the outcome of such cooperation can be seen in patients’ improved performance. Similarly, decisions on additional hearing aids, such as remote microphone and similar systems, should be made jointly between the two professionals (Drouin & Theodore, 2020).
While patient-centred interdisciplinary work is necessary for patients with a hearing impairment and no other difficulties, it becomes even more indispensable in the case of individuals with special needs, who are seen increasingly for implant interventions now that candidate selection criteria have been broadened to include people with multiple disorders. In these cases, the interdisciplinary team also has to expand to encompass other disciplines that are not usually part of an implant group. Depending on the specific disorders encountered, close collaboration may be needed with a range of professionals from neurology, neuropaediatrics, physiotherapy, occupational therapy, psychology, special education, neuropsychology, and others. In this patient group, the diagnosis itself poses enormous challenges that can only be addressed with an interdisciplinary approach. The implant decision usually requires the carefully weighed input from various professional perspectives to ensure that all variables involved are considered and to be able to provide an opinion on the outcome, adjusted as closely as possible to the patient’s individual situation. The post-operative process also requires fluid and on-going communication among the different professionals to make the necessary adjustments to deliver the most efficient auditory input possible and to help the patient gradually adapt to and use the new information received (Bavelier & Neville, 2002). These patients require more frequent adjustments and closer follow-up. Professionals should be open to trying less common alternatives, and to combining subjective and objective strategies to obtain information. In my experience, the effects of the auditory information delivered by the implant have an impact not only in the perceptual and communicative sphere, but also often drive development in other areas, fostering sensory integration that may be reflected in improved gait, basic learning mechanisms, attention, and many other aspects that favour the overall development of the individual (Nasralla et al., 2018, Corrales 2013).
Similarly, implant work with older adults should involve other professionals such as psychologists, psychiatrists and geriatricians, depending on the individual’s needs. Caregivers must also be included as an integral part of the team (Livingston et al., 2020; Sardone et al., 2019).
Patients’ parents and other relatives deserve special recognition in the part they play in team cohesion. Actively bringing them in to play a role in the process gives the team invaluable and unique insights. Children with hearing devices spend most of their time with their families, and only if the family setting shares the work objectives of the implant team can the expected benefits be achieved. Most studies that have investigated variables in cochlear implant outcomes have found that family support, family engagement in communication, and maternal educational level are three of the biggest determinants in implant outcome (Cosseti et al., 2012, Sharma et al., 2017, Boisvert 2020). It is therefore advisable that the family receives all the necessary information to ensure they are properly equipped to participate in decision-making, fully understand each phase in the process and acknowledge their role and responsibilities as integral members of the team. As in the case of well-balanced cooperation among the professional members of an interdisciplinary team, active family involvement in turn enhances the benefits of any assistive listening device, regardless of whether it is a hearing aid or a sophisticated cochlear implant.
The concept of interdisciplinarity in implant patient management is particularly conducive to comprehensive care. Interdisciplinarity orients professionals towards a holistic model of care, which aims for the overall wellbeing of the individual, moving away from the central focus on the specific goal of providing hearing health and towards facilitating cooperation in working towards a healthy life for patients (García-García & López-Torrijo, 2016; Xue et al., 2017).
Finally, it should be noted that in parallel with this harmonious cooperation among the different professionals and family, each discipline must adopt an individualised approach when caring for implant recipients, remembering that one size does not fit all. The first step is to recognise the individuality of each patient; then avoid working simply on providing a solution to a hearing problem; finally, always try to achieve a better quality of life for the patient. And this will indeed require each professional to consider the patient’s individual needs. From an audiologist’s perspective, the time spent with our patients, optimising their programming map beyond merely acceptable sound detection, will be compensated by achieving more natural, more comfortable hearing, which in turn will favour the emergence and improvement of all other aspects of a patient’s development and performance. Device manufacturers offer options today for rapid and sometimes even remote programming based on population averages and sophisticated algorithms. However, I personally believe these options should be used only in very special circumstances, because reducing the time we interact directly with our patients negatively affects the outcome, while depriving us of one of the fascinating aspects of our professional practice: sharing our knowledge with those we serve.
Conclusion
Cochlear implants have the potential to significantly change the life of recipients, their family and those in their immediate environment, with benefits that go beyond the possibility of hearing sounds, including a positive impact on the individual’s quality of life, social interactions, job opportunities, and many other aspects. Optimising the management of implant recipients by means of teamwork integrated with assertive communication among the different stakeholders involved will result in greater benefit for individuals who receive these devices to treat their hearing loss.
References
Babiker A., El Husseini M. E., Al Nemri A., Al Frayh A., Al Juryyan N., Faki M. O., Assiri A., Al Saadi M., Al Zamil F. (2014) Health care professional development: Working as a team to improve patient care. Sudan J Paedi atr; 14(2):9-16.
Bavelier D., Neville H. (2002). Cross-modal plasticity: Where and how? Nature 3:443-452.
Bernard-Bonnin A. C., Stachenko S., Bonin D., Charette C., & Rousseau, E. (1995). Self-management teaching programs and morbidity of pediatric asthma: a meta-analysis. Journal of Allergy and Clinical Immunology, 95(1), 34-41.
Boisvert I., Reis M., Au A., Cowan R., & Dowell R. C. (2020). Cochlear implantation outcomes in adults: A scoping review. PLoS One, 15(5), e0232421.
Boyle, P. (2019). Electric Stimulation of the Auditory System. https://doi.org/10.5772/intechopen.85285
Choi B. C., Pak A. W. (2006). Multidisciplinarity, interdisciplinarity and transdisciplinarity in health research, services, education and policy: 1. Definitions, objectives, and evidence of effectiveness. Clin Invest Med.; 29(6): 351-64. PMID: 17330451.
Clark, G. (2013). Cochlear implants: fundamentals and applications. Springer: New York.
Cooper H., Craddock L. (2006). Cochlear Implants: a practical guide. John Wiley & sons: Oxford.
Corrales E., Oghlai J. (2013). Cochlear Implant considerations in children with additional disabilities. Curr Otorhinolaryngol Rep. 2013 Jun 1; 1(2): 61–68.
Cosetti M. K. & Waltzman S. B. (2012). Outcomes in cochlear implantation: variables affecting performance in adults and children. Otolaryngologic Clinics of North America, 45(1), 155-171.
Dihn J., Traylor A., Kilcullen M., Perez J., Schweissing E., Venkatesh A., Salas E. (2019). Cross-Disciplinary Care: A systematic review on Teamwork processes in health Care. Small Gropu Research 51:1, 125-166.
Dorman M., Gifford R. (2017). Speech Understanding in complex listening environments by listeners fit with cochlear implants. JSLHR, 60(10), 3019-3026.
Drouin J. & Theodore R. (2020). Leveraging interdisciplinary perspectives to optimize auditory training for cochlear implant users. Lang Linguist Compass, 14:1-18.
Garcia-García F., Lopez-Torrijo M. (2016). A short communication on the need for interdisciplinary action with families with deaf children who use bilateral cochlear implants. J Med Imo Surg, 16:1-3.
Institute of Medicine Committee on the Health Professions Education Summit. (2003). The core competencies needed for health care professionals In Greiner AC & Knebel E (Eds.), Health professions education: A bridge to quality, pp. 45–74. Washington, DC: National Academies Press.
Kim L., Jeong S.W., Lee Y. M. & Kim J. S. (2010). Cochlear Implantation in children. Auris Nasus Larynx, 37(1), 6-17.
Livingston G et al. (2020). Dementia prevention, intervention and care: 2020 report of the Lancet Commission. The Lancet; 396:413-446. https://doi.org/10.1016/S0140-6736(20)30367-6
Nasralla et al. (2018). Benefit of Cochlear implantation in children with multiple handicaps: a parent’s perspective. Int Arch Otorhinolaryngol; 22:415–427.
Parikh S. R., Machleder D. J., Chobot-Rodd J., Girouard K., Shanske A., Stern E., ... & Dinces, E. (2004). Building a multidisciplinary cochlear implant team. Einstein J. Biol. Med, 21, 19-24.
Ramos-Macias A., Borkoski-Barreiro S., Falcón-González J., Ramos de Miguel A. (2016). Implante Coclear. Estado actual y futuro. Rev Med Cl Los Condes.; 27(6), 798-807.
Roderick J. L. (2010). Deciphering Interdisciplinary and Transdisciplinary Contributions. Transdisciplinary Journal of Engineering & Science; Vol: 1, No:1.
Rodríguez W. F. L., Secín D.R., Ramírez A. J. L. (2021). El trabajo en equipo como parte de un sistema de salud. Acta Med.; 19(4):477-479.
Rosen M. A., Diaz Granados D., Dietz A. S., Benishek L. E., Thompson D., Pronovost P. J., Weaver S. J. (2018). Teamwork in healthcare: Key discoveries enabling safer, high-quality care. Am Psychol.; 73(4):433-450.
Sardone R., Battista P., Panza F., Lozupone M., Griseta C., Castellana F. et al. (2019). The age-related central auditory processing disorder: silent impairment of the cognitive ear. Front Neurosci.; 13:619.
Schmutz J. B., Meier L. L., Manser T. (2019). How effective is teamwork really? The relationship between teamwork and performance in healthcare teams: a systematic review and meta-analysis. BMJ Open.
Sharma S., Bhatia K., Singh, S., Lahiri, A. K. & Aggarwal, A. (2017). Impact of socioeconomic factors on paediatric cochlear implant outcomes. International Journal of Pediatric Otorhinolaryngology, 102, 90-97.
Soskolne C. (2000). Transdisciplinary approaches for public health. Epidemiology; 11: S122.
Warner-Czyz A., Roland T., Thomas D., Uhler K., Zombek L. (2022). American Cochlear Implant Alliance task force guidelines for determining cochlear implant candidacy in children. Ear & Hear; 43, 268-282.
World Health Organization (2016). Childhood hearing loss: strategies for prevention and care. Accessed: https://www.who.int/publications/i/item/childhood-hearing-loss-strategies-for-prevention-and-care
Xue L., Le Bot G., Petegem W., van Wieringen A. (2017). Defining interdisciplinary competencies for audiological rehabilitation: findings from a modified Delphi study, Int Jour Audiol; 1-12.
Ysunza A (2014). Audiologia, Otoneurologìa y Foniatría, la más interdisciplinaria especialidad médica. Rev Mex AMCAOF; 3: 5-6.
Zaltz Y., Bugannim Y., Zechoval D., Kishon-Rabin L., Perez R. (2020). Listening in Noise Remains a Significant Challenge for Cochlear Implant Users: Evidence from Early Deafened and Those with Progressive Hearing Loss Compared to Peers with Normal Hearing. J Clin Med.; May 8;9(5):1381.
Zajac S., Woods A., Tannenbaum S., Salas E. and Holladay C. L. (2021). Overcoming Challenges to Teamwork in Healthcare: A Team Effectiveness Framework and Evidence-Based Guidance. Front. Commun., 17 March 2021, v. 6. https://doi.org/10.3389/fcomm.2021.606445
Conflict of interest
The author declares no conflicts of interest.
How to cite
Barón de Otero, C. (2024).
Interdisciplinary work: essential for optimising hearing implant outcomes. Auditio, 8, e91.
https://doi.org/10.51445/sja.auditio.vol8.2024.0091
Correspondence
Clemencia Barón de Otero
Instituto Nacional de Otología García
Gómez, Bogotá, Colombia.
email: clemenciabaronc@gmail.com
Editorial Office
Copyeditor: Tomás Pérez Pazos
Translation: Emma Goldsmith
Trans. Revision: Helia Relaño-Iborra
Production: Glaux Publicaciones Académicas